What Is the Highest Rating a Blood Co2 Machine Reads
Sympathise how monitoring end-tidal carbon dioxide helps assess and treat a patient in respiratory distress
Respiratory distress is ane of the most common patient complaints. Waveform capnography is a valuable tool to determine the cause and severity of respiratory distress, to guide treatment decisions, and to monitor the patient's response to treatment. Here are five things you should know about capnography and respiratory distress:
1. The shape of the capnography waveform helps decide the cause of the trouble
Authentic diagnosis of the cause of respiratory distress is disquisitional, but can be difficult when the patient has difficulty speaking or multiple chronic respiratory conditions. Diminished breath sounds, wheezes, and crackles can be caused past multiple conditions, including asthma, COPD, CHF and pneumonia. When added to a thorough history and physical exam, waveform capnography is a valuable assessment tool.
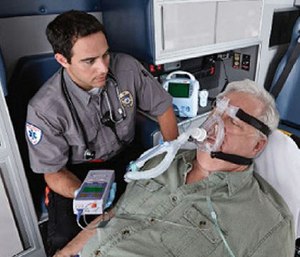
The shape of the capnography waveform represents air movement through the lungs, similar to how an ECG tracing represents electric activity in the heart. Capnography is measured with an adapter between the purse-valve device and the mask, or with nasal prongs that sample exhaled air from the rima oris and nose. The waveform begins at baseline when exhaled air from the dead space in the upper airway reaches the sensor, which contains no measurable CO2. A spike is seen when CO2-filled air released from the alveoli first passes the olfactory organ and lips, and then plateaus when all air is exhaled from the alveoli. The waveform then slopes downward at the beginning of inhalation and returns to baseline. A normal waveform is rectangular shaped, with a slight meridian during the plateau.
With bronchoconstriction, acquired by asthma, COPD, and sometimes pneumonia, air is released inconsistently from the constricted lower airways. This causes the normally rectangular-shaped capnography waveform to take a "shark-fin" appearance [1].
Bronchoconstriction may also crusade a longer expiratory phase, seen as a longer waveform. The more pronounced the shark fin and the longer the exhalation phase, the more constricted the lower airways are. A nebulized bronchodilator, such every bit albuterol, is indicated when patients accept a shark-fin waveform and bronchoconstriction to open lower airways and increment air movement.
A rectangular-shaped waveform ways that there is no constriction of the lower airways, and that there must exist another cause of the patient's respiratory distress. These causes include fluid in the alveoli, such as from CHF, and excessive mucus secretion in the lower airways, such from pneumonia or bronchitis. While both compromise air commutation and increase the attempt needed to breathe, air still leaves the alveoli consistently and generates a rectangular capnography waveform. A nebulized bronchodilator would not help, and may harm, respiratory conditions not caused by bronchoconstriction. A rectangular capnography waveform means that there is no bronchoconstriction, and that no bronchodilator is needed.
2. Think respiratory failure when ETCO2 is high
Capnography adds objective data to physical exam findings, which helps make up one's mind the severity of respiratory distress. CO2 is a byproduct of cellular metabolism, which gets transported in the blood to the lungs for elimination. The corporeality of CO2 at the end of exhalation, or finish-tidal CO2 (ETCO2) is normally 35-45 mm HG. The height of the capnography waveform accompanies this number on the monitor, as well as the respiratory rate.
In severe cases of respiratory distress, increased effort to exhale does not effectively eliminate CO2. This causes CO2 to accrue in the lungs and more of information technology to be excreted with each jiff (hypercapnea), which would cause the ETCO2 level to ascent.
Increased work of breathing and CO2 retention may somewhen lead to respiratory arrest and assisted ventilation is needed. Respiratory failure from fatigue may occur even when patients inhale plenty oxygen, thus having a normal pulse-ox reading. High ETCO2 helps predict respiratory arrest before a change in mentation and decompensation occur, and time to ready airway equipment.
3. Think perfusion, metabolic or psychological problem when ETCO2 is low
Other respiratory weather can cause a depression ETCO2 reading or hypocapnea. With pulmonary embolism, a blocked pulmonary artery causes less CO2-rich claret to render to the lungs, and less CO2 is released with each breath. Diabetic ketoacidosis (DKA) may present with difficulty breathing, rapid respiratory charge per unit, and depression ETCO2 as the trunk attempts to compensate for acidosis [ane].
Shortness of jiff from anxiety-induced hyperventilation is caused by an excess of CO2 exhalation. While this is a common and benign status, its presentation, ETCO2, and capnography waveform is like to more than serious conditions. While coaching the patient to slow their animate may help better symptoms when anxiety is the suspected crusade of hyperventilation and increased ETCO2, information technology is of import to appraise for other weather condition. Follow your local protocols for transport of patients with anxiety-induced hyperventilatoin.
4. Capnography provides real-time feedback on response to handling
A decrease in respiratory rate, effort, and anxiety level are signs of both improvement and worsening respiratory failure. Waveform capnography helps make a definitive decision to guide further treatment.
The shark-fin waveform changes to a rectangular shape if the patient responds well to a animate treatment. Other medications, such every bit epinephrine or magnesium sulfate, may be needed if the shark fin does not change or becomes more pronounced.
For patients who present with a loftier ETCO2 reading, a subtract with treatment indicates that they are getting meliorate. No change or a rising ETCO2 level indicates that respiratory effort is still failing to adequately eliminate CO2, and that more other interventions are needed. A patient receiving supplemental oxygen may need CPAP, and patients whose ETCO2 rises with CPAP may need assisted ventilation with a BVM.
5. Hyperventilation with a BVM is harmful, and capnography can help forbid it
While increasing ETCO2 is a sign of respiratory failure, patients can tolerate hypercapnea for long periods one time ventilation is assisted [2]. Correction of hypercapnea while receiving mechanical ventilation is a complicated process that must be done in the hospital. Hypoxia is a true emergency, just hyperventilation with a BVM does not assistance correct it faster.
Hyperventilation with a BVM is harmful because it does not allow plenty time for exhalation, which worsens air trapping from bronchoconstriction and tin can cause lung injury. Hyperventilation as well increases intrathoracic pressure, which increases the workload of the eye [two]. This is especially harmful in CHF patients whose cardiac output is already compromised.
Waveform capnography has been shown to reduce the incidence of hyperventilation [3]. Each squeeze of the BVM generates a waveform and displays feedback on respiratory charge per unit. Use ETCO2 equally a guide to ventilate patients ten-12 times per minute, and deliver only enough tidal book needed to make the breast rise. It is too of import to allow patients to exhale completely before delivering the side by side ventilation – fifty-fifty if the respiratory charge per unit must be lower to accomplish this – which tin be monitored by viewing the length of the capnography waveform.
Waveform capnography is a reliable tool to assess the cause and severity of respiratory distress. Use it to help make authentic handling decisions and adapt to condition changes.
Read next: Capnography in Ems: Tube verification is only the beginning
References
- Kraus B. Advances in the use of capnography for non-intubated patients. Israeli Journal of Emergency Medicine 2008; 8 (iii) three-15.
- Vanden Hoek TL, Morrison LJ, Shuster M, et al. Part 12: cardiac arrest in special situations. 2010 American Heart Association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation 2010; 122 (suppl 3): S829-S861.
- Davis DP, Dunford JV, Ochs M, et al. The use of quantitative end-tidal capnometry to avert inadvertent severe hyperventilation in patients with head injury after paramedic rapid sequence intubation. J Trauma 2004; 56(4):808-814, Apr 2004.
This commodity was posted Oct. 13, 2015. Information technology has been updated.
Most the author
Bob Sullivan, MS, NRP, is a paramedic instructor at Delaware Technical Community College and works as a field provider in the Wilmington, Del. area. He has been in European monetary system since 1999, and has worked as a paramedic in private, fire-based, volunteer and municipal Ems services. Contact Bob at his blog, EMS Theory to Practise.
What Is the Highest Rating a Blood Co2 Machine Reads
Source: https://www.ems1.com/ems-products/capnography/articles/5-things-to-know-about-capnography-and-respiratory-distress-6NhW3UN9TSPk4X2I/